Connect With Us
Featured Articles
Items filtered by date: December 2019
Morton's Neuroma
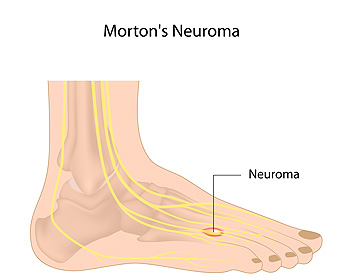
A neuroma is a thickening of nerve tissue and can develop throughout the body. In the foot, the most common neuroma is a Morton’s neuroma; this typically forms between the third and fourth toes. The thickening of the nerve is typically caused by compression and irritation of the nerve; this thickening can in turn cause enlargement and, in some cases, nerve damage.
Neuromas can be caused by anything that causes compression or irritation of the nerve. A common cause is wearing shoes with tapered toe boxes or high heels that force the toes into the toe boxes. Physical activities that involve repeated pressure to the foot, such as running or basketball, can also create neuromas. Those with foot deformities, such as bunions, hammertoes, or flatfeet, are more likely to develop the condition.
Symptoms of Morton’s neuroma include tingling, burning, numbness, pain, and the feeling that either something is inside the ball of the foot or that something in one’s shoe or sock is bunched up. Symptoms typically begin gradually and can even go away temporarily by removing one’s shoes or massaging the foot. An increase in the intensity of symptoms correlates with the increasing growth of the neuroma.
Treatment for Morton’s neuroma can vary between patients and the severity of the condition. For mild to moderate cases, padding, icing, orthotics, activity modifications, shoe modifications, medications, and injection therapy may be suggested or prescribed. Patients who have not responded successfully to less invasive treatments may require surgery to properly treat their condition. The severity of your condition will determine the procedure performed and the length of recovery afterwards.
Morton’s Neuroma and Pinched Nerves
A pinched nerve that is located between the toes may be referred to as Morton’s Neuroma. It may occur as a result of an injury that happened to the foot, and the pain that is felt is generally on the ball of the foot as it radiates from the toes. When a diagnosis is performed, the range of motion is checked, and this is helpful in looking for arthritis or inflamed joints. Additionally, it is important that an X-ray or MRI is performed, as this may be beneficial in ruling out other ailments. Moderate relief may be found when the correct shoes are worn, and it may help to add support to the affected area by taping the foot. If you are afflicted with Morton’s Neuroma, it is advised that you speak to a podiatrist who can guide you toward the proper treatment, which may include surgery.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Howard Horowitz of Bowie Foot & Ankle . Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Bowie, MD. We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Morton's NeuromaMorton's Neuroma
A neuroma is a thickening of nerve tissue and can develop throughout the body. In the foot, the most common neuroma is a Morton’s neuroma; this typically forms between the third and fourth toes. The thickening of the nerve is typically caused by compression and irritation of the nerve; this thickening can in turn cause enlargement and, in some cases, nerve damage.
Neuromas can be caused by anything that causes compression or irritation of the nerve. A common cause is wearing shoes with tapered toe boxes or high heels that force the toes into the toe boxes. Physical activities that involve repeated pressure to the foot, such as running or basketball, can also create neuromas. Those with foot deformities, such as bunions, hammertoes, or flatfeet, are more likely to develop the condition.
Symptoms of Morton’s neuroma include tingling, burning, numbness, pain, and the feeling that either something is inside the ball of the foot or that something in one’s shoe or sock is bunched up. Symptoms typically begin gradually and can even go away temporarily by removing one’s shoes or massaging the foot. An increase in the intensity of symptoms correlates with the increasing growth of the neuroma.
Treatment for Morton’s neuroma can vary between patients and the severity of the condition. For mild to moderate cases, padding, icing, orthotics, activity modifications, shoe modifications, medications, and injection therapy may be suggested or prescribed. Patients who have not responded successfully to less invasive treatments may require surgery to properly treat their condition. The severity of your condition will determine the procedure performed and the length of recovery afterwards.
Morton’s Neuroma and Pinched Nerves
A pinched nerve that is located between the toes may be referred to as Morton’s Neuroma. It may occur as a result of an injury that happened to the foot, and the pain that is felt is generally on the ball of the foot as it radiates from the toes. When a diagnosis is performed, the range of motion is checked, and this is helpful in looking for arthritis or inflamed joints. Additionally, it is important that an X-ray or MRI is performed, as this may be beneficial in ruling out other ailments. Moderate relief may be found when the correct shoes are worn, and it may help to add support to the affected area by taping the foot. If you are afflicted with Morton’s Neuroma, it is advised that you speak to a podiatrist who can guide you toward the proper treatment, which may include surgery.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Howard Horowitz of Bowie Foot & Ankle . Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Bowie, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Why Does Plantar Fasciitis Occur?
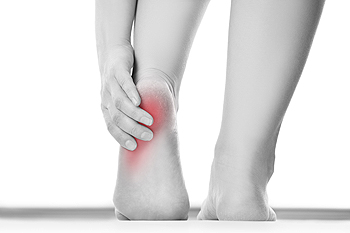 A common foot condition that affects numerous patients is referred to as plantar fasciitis. This occurs when the tissue that is located on the bottom of the foot becomes inflamed. This condition focuses on the plantar fascia, which connects the toes to the heels. The arch is supported by this band of tissue, and can be affected as this condition progresses. There are common reasons why plantar fasciitis may gradually develop. These can consist of standing for the majority of the day, existing foot conditions that may include having a rigid Achilles tendon, and wearing shoes that do not fit correctly. Patients may find moderate relief when the affected foot is elevated. It may also be beneficial to perform exercises that can strengthen the overall foot. Additionally, it may help to tape the foot which can provide support. If you feel you have this ailment, it is suggested that you schedule a consultation with a podiatrist who can help you to manage this condition.
A common foot condition that affects numerous patients is referred to as plantar fasciitis. This occurs when the tissue that is located on the bottom of the foot becomes inflamed. This condition focuses on the plantar fascia, which connects the toes to the heels. The arch is supported by this band of tissue, and can be affected as this condition progresses. There are common reasons why plantar fasciitis may gradually develop. These can consist of standing for the majority of the day, existing foot conditions that may include having a rigid Achilles tendon, and wearing shoes that do not fit correctly. Patients may find moderate relief when the affected foot is elevated. It may also be beneficial to perform exercises that can strengthen the overall foot. Additionally, it may help to tape the foot which can provide support. If you feel you have this ailment, it is suggested that you schedule a consultation with a podiatrist who can help you to manage this condition.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Howard Horowitz from Bowie Foot & Ankle . Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Bowie, MD. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Plantar FasciitisPlantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Why Does Plantar Fasciitis Occur?
 A common foot condition that affects numerous patients is referred to as plantar fasciitis. This occurs when the tissue that is located on the bottom of the foot becomes inflamed. This condition focuses on the plantar fascia, which connects the toes to the heels. The arch is supported by this band of tissue, and can be affected as this condition progresses. There are common reasons why plantar fasciitis may gradually develop. These can consist of standing for the majority of the day, existing foot conditions that may include having a rigid Achilles tendon, and wearing shoes that do not fit correctly. Patients may find moderate relief when the affected foot is elevated. It may also be beneficial to perform exercises that can strengthen the overall foot. Additionally, it may help to tape the foot which can provide support. If you feel you have this ailment, it is suggested that you schedule a consultation with a podiatrist who can help you to manage this condition.
A common foot condition that affects numerous patients is referred to as plantar fasciitis. This occurs when the tissue that is located on the bottom of the foot becomes inflamed. This condition focuses on the plantar fascia, which connects the toes to the heels. The arch is supported by this band of tissue, and can be affected as this condition progresses. There are common reasons why plantar fasciitis may gradually develop. These can consist of standing for the majority of the day, existing foot conditions that may include having a rigid Achilles tendon, and wearing shoes that do not fit correctly. Patients may find moderate relief when the affected foot is elevated. It may also be beneficial to perform exercises that can strengthen the overall foot. Additionally, it may help to tape the foot which can provide support. If you feel you have this ailment, it is suggested that you schedule a consultation with a podiatrist who can help you to manage this condition.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Howard Horowitz from Bowie Foot & Ankle . Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Bowie, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What is a Podiatrist?
The branch of medicine that is focused on the treatment, diagnosis, and study of disorders of the lower leg, ankle and foot is referred to as podiatry. Because people often spend a great deal of their time on their feet, many problems in this area can occur. A person seeks help from the field of podiatry when they need treatment for heel spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems, infections, and problems with the foot that are related to diabetes and additional diseases.
To treat problems of the foot, ankle or lower leg, a podiatrist may prescribe physical therapy, drugs, perform surgery, or set fractures. Individuals may also be recommended to wear corrective shoe inserts, custom-made shoes, plaster casts and strappings in order to correct deformities.
When trying to gather information on a patient problem, a scanner or force plate may be used in order to design orthotics. During this procedure, patients are told to walk across a plate that is connected to a computer; the computer then takes a scan of the foot and indicates weight distribution and pressure points. The computer readouts will give the podiatrist information to help them determine the correct treatment plans.
Diagnosis is also provided through laboratory tests and x-rays. Through the foot, the first signs of serious problems such as heart disease, diabetes and arthritis can show up. For example, individuals that have diabetes may frequently have problems such as infections and foot ulcers because they experience poor circulation in the foot area. A podiatrist can then have consultations with patients when symptoms arise. Referrals will then be made to specialists that handle the greater health problems.
Some podiatrists have their own independent, private practices or clinics where they have a small staff and administrative personnel. Many podiatrists work within group practices. They usually spend time performing surgery in ambulatory surgical centers or hospitals, or visit patients in nursing homes. Podiatrists typically spend between 30 to 60 hours of week working. Some podiatrists specialize in public health, orthopedics, surgery, or primary care. Other fields include specialties in geriatrics, dermatology, pediatrics, diabetic foot care and sports medicine.
Some podiatrist specialists complete extra training in the area of foot and ankle reconstruction that results from the effects of physical trauma or diabetes. There are also surgeons that perform surgery of a cosmetic nature to correct bunions and hammertoes.
Levels of School for Podiatrists
 People who have the desire to learn about the treatment and prevention of foot disorders may work in the field of podiatry. They learn about how the foot is constructed, and the importance of maintaining proper foot care. The levels of education consist of earning a bachelor's degree, followed by enrolling in a college of podiatric medicine. This is a four year program, and incorporates two years of laboratory work. Upon completion, the student will become a doctor of podiatric medicine, which is referred to as a DPM. Residency training provides the skills needed to perform a variety of foot surgeries, in addition to learning about different medical techniques. If you are interested in pursuing a career in podiatry, it is advised that you confer with a podiatrist who can guide you in determining if this is a correct choice for you.
People who have the desire to learn about the treatment and prevention of foot disorders may work in the field of podiatry. They learn about how the foot is constructed, and the importance of maintaining proper foot care. The levels of education consist of earning a bachelor's degree, followed by enrolling in a college of podiatric medicine. This is a four year program, and incorporates two years of laboratory work. Upon completion, the student will become a doctor of podiatric medicine, which is referred to as a DPM. Residency training provides the skills needed to perform a variety of foot surgeries, in addition to learning about different medical techniques. If you are interested in pursuing a career in podiatry, it is advised that you confer with a podiatrist who can guide you in determining if this is a correct choice for you.
If you are experiencing pain in the feet or ankles, don’t join the stubborn majority refusing treatment. Feel free to contact Dr. Howard Horowitz from Bowie Foot & Ankle . Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Podiatrist?
Someone would seek the care of a podiatrist if they have suffered a foot injury or have common foot ailments such as heal spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems, etc.
Podiatric Treatment
A podiatrist will treat the problematic areas of the feet, ankle or lower leg by prescribing the following:
- Physical therapy
- Drugs
- Orthotic inserts or soles
- Surgery on lower extremity fractures
A common podiatric procedure a podiatrist will use is a scanner or force plate which will allow the podiatrist to know the designs of orthotics. Patients are then told to follow a series of tasks to complete the treatment. The computer will scan the foot a see which areas show weight distribution and pressure points. The podiatrist will read the analysis and then determine which treatment plans are available.
If you have any questions please feel free to contact our office located in Bowie, MD. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about What is a Podiatrist?